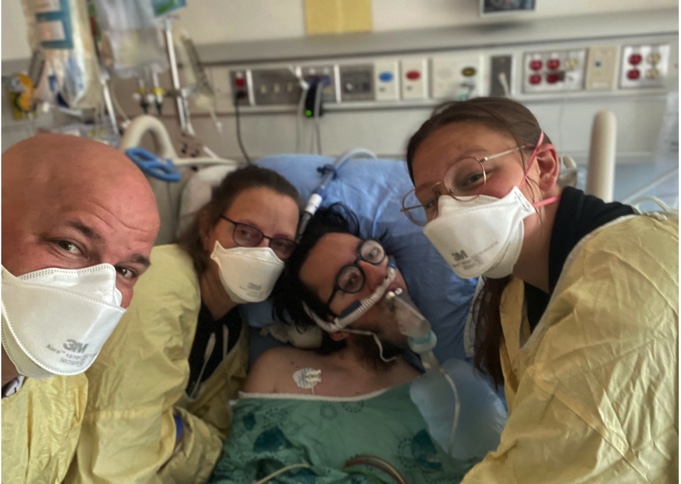
Deane was supposed to be at camp this week, hanging with his friends, chatting with the cute counsellors. He was going to be a junior “nurse’ this session.
Instead, he is intubated and sedated in an out-of-town hospital.
Five days ago, Deane woke up late at the cottage, groggy and definitely not himself. Checking his blood oxygen level with an oximeter we bought after my recent bout of pneumonia, we found it was dangerously low. He was also running a slight fever. After a short ambulance ride to the small local hospital followed by a longer ambulance ride to the regional hospital, Deane was admitted to the ICU with a serious case of pneumonia.
Immediately the team got to work stabilizing Deane. Heavy duty nasal prongs were insufficient because much of the oxygen they delivered flowed out of his always-open mouth. They did not have a mask large enough to cover both his mouth and nose so they improvised with the prongs and a mask over his mouth. They did a deep suction with a camera which confirmed what earlier X-rays showed: Deane’s left and part of his right lungs had collapsed.
At 4 a.m., 24 hours after being admitted, the team is struggling to maintain Deane’s oxygen levels. Enter a doctor who said rather bluntly, that intubation and likely a tracheostomy would be the solution.
I know it is the middle of the medical team’s day, but having a doctor come in and inform me that there was a real possibility a hole would be put in my son’s throat when I was operating on 90 minutes of sleep beside Deane’s bed after a stressful day of trying get my daughter and me to an unfamiliar town to support Deane and my husband from a hotel room, was not something I wanted to hear. The ability to absorb information like that in the middle of the night is a skill I wish I had never had to learn.
After the scope, Deane had 75% capacity in his left lung. For the rest of the night, there was little improvement. In the morning, the doctor came in and said mucus and secretions were still building up in Deane’s lungs so they were going to intubate him. It was a different doctor, same discussion: if he didn’t improve with the intubation we should consider a tracheostomy. Deane is going to continue to struggle with secretions, he said, continue to get pneumonia and will need a trach sooner or later.
My husband, trying to start a work day from the hotel, and my daughter, just out of the shower, rushed to the hospital. With an exception to the visiting rules, we were all allowed to be in the room with Deane, making him laugh and hearing him answer questions with his enthusiastic, sparkling-eyed “Yeah.” My daughter and I left, knowing intubation was the right decision, and allowing my husband to walk Deane through what was about to happen.
Once Deane was completely sedated, the three of us reconvened in one of those awkward family waiting rooms with hugs and tears.
Earlier this week, the doctor said to my husband, “You’ve done an incredible job keeping him this healthy for 24 years.” It’s always nice to a get a compliment, even in these circumstances. Now it is the doctor’s turn – along with Deane’s determination – to get him healthy again.
Discussion
No comments yet.